What Is Normal For You Lady Parts After Childbirth
I posted a question in my Instagram stories, asking what was something that you wanted to know or wish you had known about pelvic health after pregnancy.
The most common question was, what is normal and what’s not for your lady parts after giving birth?
That’s a big one, and to be honest, these were things I didn’t know my first time around.
What I’m about to chat about now will save a lot of confusion, and it will empower you to move forward your fitness journey.
Not hold you back.
After my second pregnancy, I was diagnosed with a grade two prolapse. My main symptom was peeing myself during workouts. Mostly when jumping and running.
The most common culprits known to make women a little leaky during their workouts.
Most women believe this to be a normal part of giving birth or chalking it up to working really hard during exercise.
You don’t have to put up with peeing when you’re not in the bathroom. For most women, accidentally peeing their pants can be managed. You don’t have to make frequent bathroom trips during your workouts or at any point during your day.
What may be normal for you,
This is more common than you think. With 1-3 women experiencing something happening with her pelvic floor, more women are moving away from shame and feeling hopeful with education and support.
First, here are the most common symptoms women experience in their lady parts.
Stress Urinary Incontinence
This is where you pee when you laugh, sneeze, cough, and exercise.
Many women find this happens more so after having a baby, but young female athletes experience this, too.
This common occurrence happens for various reasons, like:
- Weak pelvic floor muscles
- Overactive pelvic floor muscles
- How the air in the belly (Intra Abdominal pressure IAP), is managed when force is placed on it.
- Caffeine or other bladder irritants and diuretics
Learning how to manage IAP and finding your pee free zone during exercise will be a big help in reducing your chances of peeing when you’re not in the bathroom.
And it isn’t just about the leaks during your workouts, it’s about why and when they’re happening. Here are some questions you can ask yourself.
- Is it just in explosive activity?
- Is it only when you lift heavy?
- What does your alignment look like?
- Are your ribs shifted behind your pelvis?
- How are you landing during those jumps?
- What does your alignment look like when you’re running?
There are a lot of questions that I’ll ask, because peeing during your workouts may not indicate that there’s really a pelvic floor dysfunction or disorder.
It just may mean you need to look at how you’re managing the air in your belly, known as
If there’s some breath-holding during those movements, that may contribute to pressure. Overall, the idea is to minimize the leaking as much as you can, if it’s related to IAP.
You can do this by contracting your pelvic floor (pulling it up and in) as you exert during the movement.
Urge Incontinence
This is the sudden onset of “I gotta go and I gotta go now”.
You may have also heard some refer it to an overactive bladder. Basically, it’s the bladder staying relaxed as it fills up. And for some, the bladder contracts sooner than it needs to and may feel fuller than it is.
I don’t deal with urge incontinence as a coach, so there isn’t a lot of detail in this article. But if you are experiencing this, consult with your doctor and get assessed by a pelvic PT.

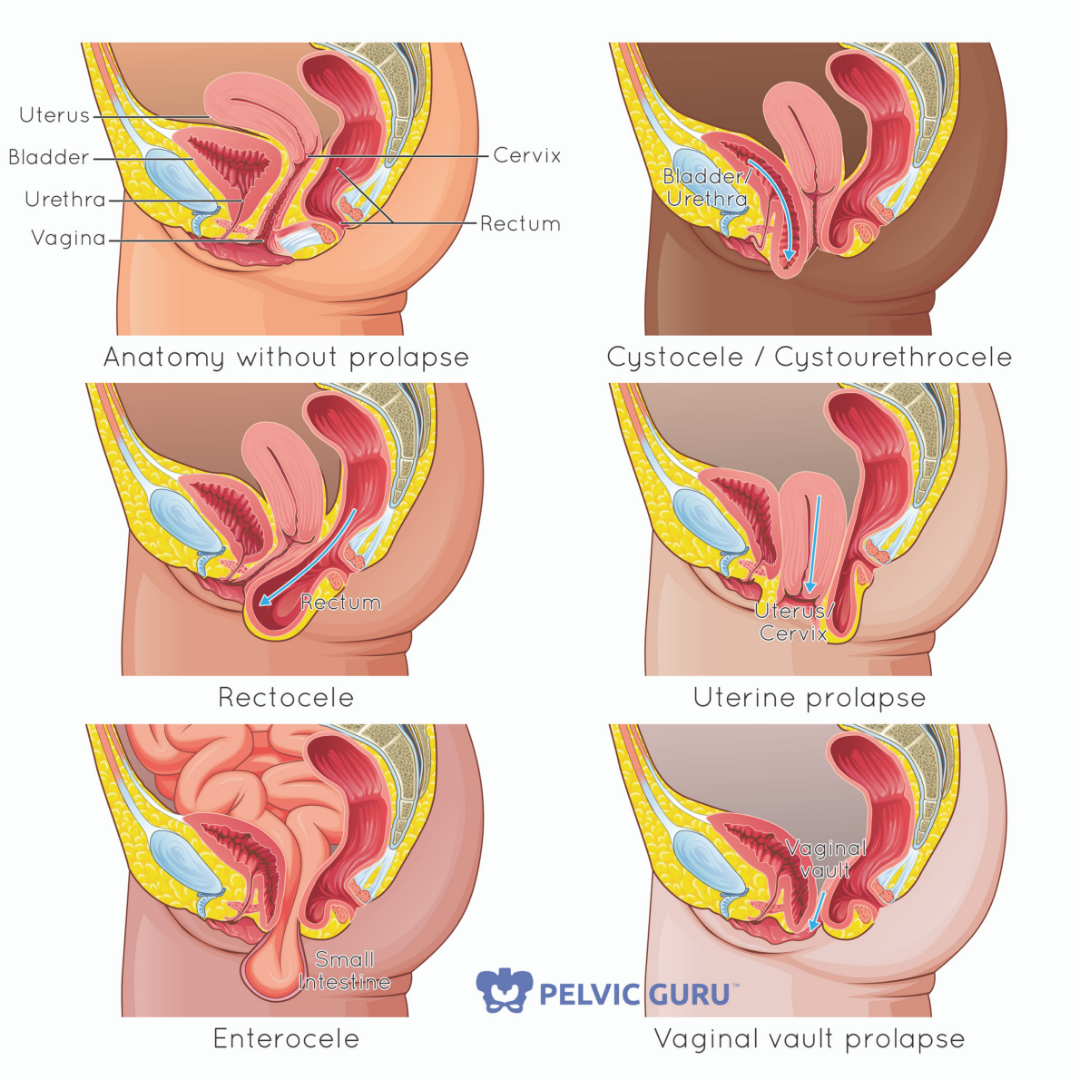
Pelvic Organ Prolapse (POP)
POP is where one or more of your pelvic organs bulge through your vagina. This doesn’t mean your organs are going to come out of your lady parts. It means these organs are bulging through your vaginal vault.
After the birth of my second child, I was diagnosed with
In, From Prolapse To Proud And Powerful, I share how I overcame my fears of POP to sign myself up to the most intensive fitness programming on the planet, CrossFit without experiencing a single symptom.
So if you’ve had a c-section, this doesn’t mean your lady parts are off the hook.
At this point, I’m symptom-free for the most part, but I’ve learned to manage my symptoms with pelvic floor rehab and strength training.
Some women
Other Common Symptoms of Pelvic Organ Prolapse?
- A feeling of pressure or fullness in the pelvic area.
- A backache low in the back.
- Pain/discomfort during sexual activity.
- A feeling that something is falling out of the vagina.
- Urinary problems such as leaking of urine or a chronic urge to urinate.
- Constipation.
You may find symptoms creep up depending on where you are in your cycle, times of stress and lack of sleep, or times of hormonal shifts like pregnancy, breastfeeding, and (peri)menopause.
If you’re experiencing symptoms like these, a pelvic PT can help. And not to worry, you can continue your workouts and learn to manage symptoms with online fitness programs like Strength And Lady Parts
Permission to use copyright image from Pelvic Guru, LLC
Pain Inside Or Outside Your Lady Parts
Let’s talk about pain. If you feel pain in your pelvic floor, inside of your vagina, or outside known as the vulva, this can be treated by a pelvic floor physiotherapist.
We shouldn’t be experiencing pain anywhere really in our bodies, and it could be due to a number of different reasons.
Some women experience pain upon penetration, that could be an indication of:
- An overactive pelvic floor.
- Scar tissue from an episiotomy or tearing during a vaginal delivery
- Anxiety about sex. This may be something to work through with a pelvic PT and a therapist.
Sex really shouldn’t be painful, it should feel good.
Pain outside of the vagina, in the vulva, this is a very important piece to our pelvic health, and it can be treated. Again, this can happen for a number of different reasons.
I don’t address vulvodynia (pain within the vulva), or vaginismus (pain inside the vagina. That would be an automatic referral to a pelvic floor physiotherapist.
Pain During And Post-Workout Or Activity
The most common pelvic health symptoms I see with my clients is pain during and/or post-workouts or activity. This means you may have pain when pushing your kiddos in their stroller or while you’re grocery shopping.
Typically, what I see is the pelvic floor is working hard during high impact training. This can be lifting heavy weights, running, or sports where you’re changing direction quickly like soccer.
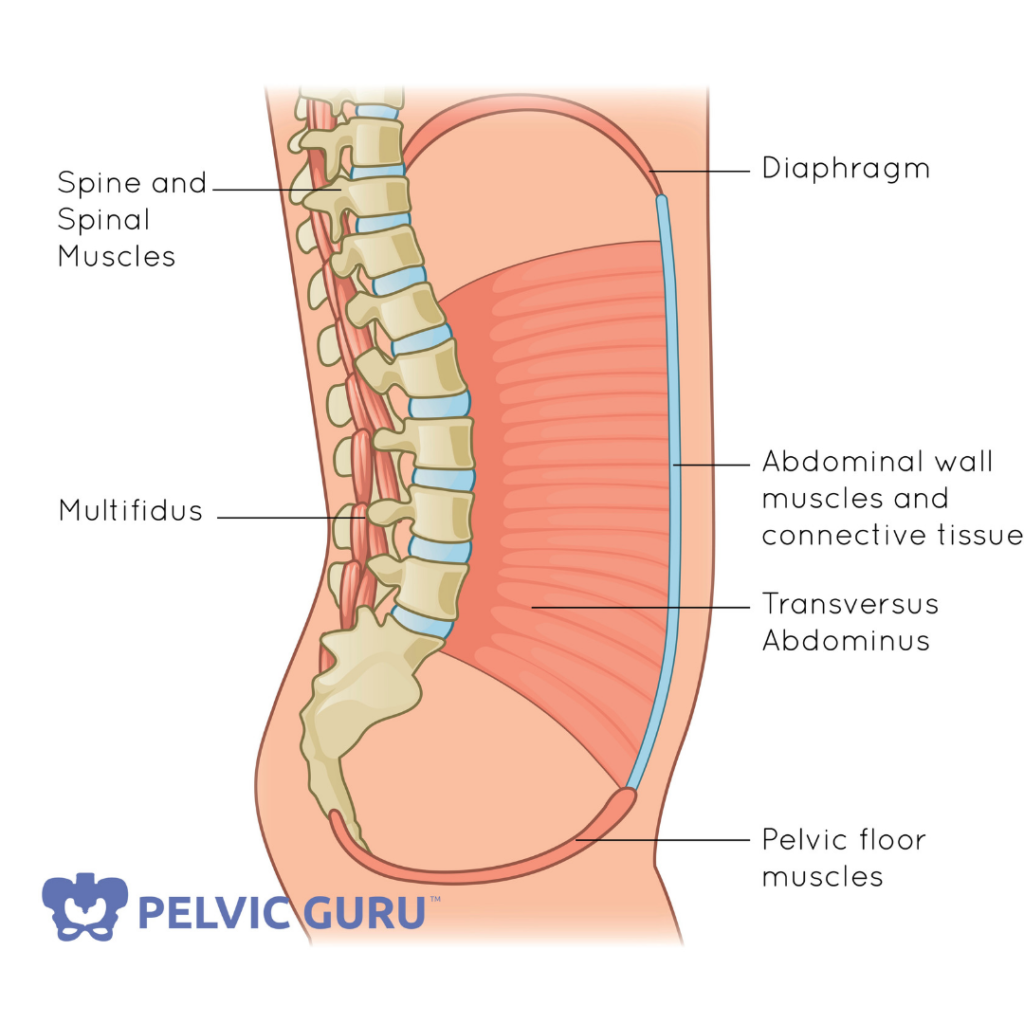
With weightlifting, your pelvic floor is in overdrive to support the demands of the heavy lift. Yes, your vaginal muscle activate as they are a part of your deep core system (diaphragm, pelvic floor, multifidus, and transversus abdominis TVA)
Permission to use copyright image from Pelvic Guru, LLC
And with running and jarring movement like changing your direction quickly, your pelvic floor isn’t given the chance to relax and contract.
So you may find pain or discomfort within your lady parts because your pelvic floor is like any other muscle. It works hard and gets tired.
Learning to relax, or open these muscles during and post-workout will ease some of the tension.
First, start with your breathing as a part of your cool down.
- Inhale deeply through your nose
- Exhale through your mouth and visualize your vagina opening
- Repeat for 1-5 minutes with every exhale, your vagina opening a bit more every time.
Learning how to work within your symptom free zone doesn’t mean you’ll be stuck there forever. You can increase intensity as your pelvic floor adapts to the impact placed on it.
It might be that all you need is just a small little tweak in your strategy or you may need to learn how to manage your symptoms during your workouts using a program like Strength And Lady Parts.
Take your symptoms as feedback, not a contraindication of exercise.
If you have symptoms during your first rep, you may want to put your detective hat on and investigate it by checking alignment, breathing, and overall strategy like I talk about above.
If you’re experiencing it towards the end of your workout, it generally indicates fatigue.
What Next?
Many women have been able to return to high impact training by learning to manage their symptoms.
And If you are in a fitness class, working with a coach one on one, and you’re leaking, experiencing pain in your lady parts, or feel a bulge “hey, coach, I have symptoms” and they should help you find modifications right for you. Remember, if you’re not comfortable sharing your symptoms, you can ask for modification options. You don’t have to divulge what’s happening down below in a room full of people.
Buuuuut, this is valuable information your coach needs to know. Speak to them in a private setting if that makes you more comfortable.
I hate to use the terms “normal” and “not normal” because that could bring up a fear in terms of how we see our bodies. And you may find your normal is different than someone else’s.
You need to look at is what’s normal for you.
In Strength And Lady Parts, my online strength and conditioning for women, you will build a strong foundation for your pelvic health as well as learn how to manage your pelvic floor symptoms like peeing during your workouts, pelvic floor pain as well as pelvic organ prolapse.
If you’re looking to up the ante in your training with your pelvic floor in mind, tap here to learn more..
Don’t Let Your Pelvic Floor Keep You From The Activities You Love…Including Sex!
Take the first steps in managing your pelvic floor dysfunctions by grabbing your free copy of my 10 Fitness Tips For Your Lady Parts: A 10 Step Checklist To Improve Your Pelvic Health.
You will learn the ins and outs of core training improve your pelvic floor function, how to optimize your sleep and stress management (yep, sleep and stress have an impact on your pelvic floor, too), and the functional movements you need to build full body strength to maximize your training results. Click on the button below to grab your free 10 step checklist now.
Resources:
-
Relevance of open magnetic resonance imaging position (sitting and standing) to quantify pelvic organ prolapse in women.Abdulaziz M1, Kavanagh A2, Stothers L3, Macnab A2,3. https://www.ncbi.nlm.nih.gov/pubmed/29989885
-
Positional pelvic organ prolapse (POP) evaluation using open, weight-bearing magnetic resonance imaging (MRI).Friedman B1, Stothers L2, Lazare D3, Macnab A2. https://www.ncbi.nlm.nih.gov/pubmed/26225170
- Pelvic floor muscle activity in different sitting postures in continent and incontinent women. Sapsford RR1, Richardson CA, Maher CF, Hodges PW. https://www.ncbi.nlm.nih.gov/pubmed/18760158
- Symptomatic pelvic organ prolapse and possible risk factors in a general population. Am J Obstet Gynecol. 2009 Feb;200(2):184.e1-7.

